While we have made an effort to ensure that this information is correct and current, the law is regularly changing, and we cannot guarantee the accuracy of the information provided. This information may not be applicable to your specific situation and is not, and should not be relied upon, as a substitute for legal advice.
HIV-Specific Criminal Laws
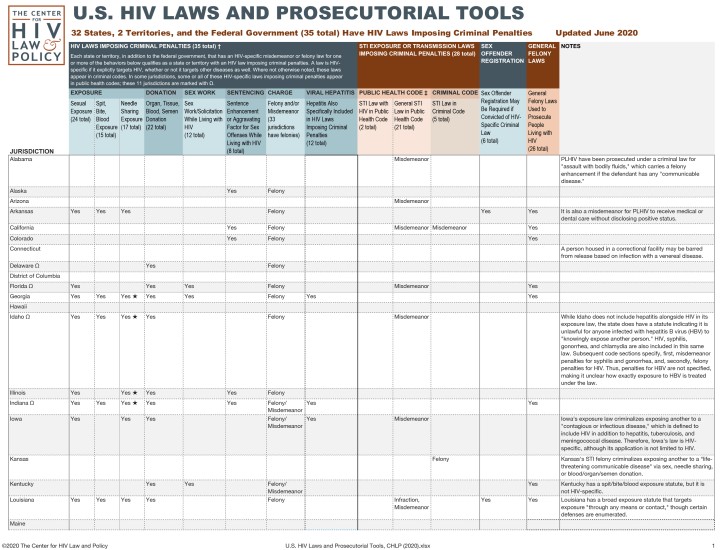
There are no criminal statutes explicitly addressing HIV exposure in Rhode Island.
For detail on the selected state law and cases interpreting it, see Rhode Island: Analysis & Codes, an excerpt from CHLP’s recently updated compendium of HIV- and STI-related criminal laws and civil laws relating to public health control measures in all 50 states, the military, and U.S. territories. To view the publication in its entirety, see HIV Criminalization in the United States: A Sourcebook on State and Federal HIV Criminal Law and Practice. Methodology is explained in the Introduction (page 5).
A person with an STI may be charged with a misdemanor for exposing others to disease.
State Guidelines on Health Care Workers with HIV
We currently are in the process of reviewing and updating our resources and summaries related to health care workers and disclosure. In the meantime, please do not rely on this information as current, and get in touch with CHLP with any questions.
Voluntary
Whether infected HCW will be required to prospectively notify patients in order to perform certain procedures will be judged on a case-by-case basis.
Review of infected HCW will be based on premise that infection alone does not justify limiting HCW’s duties. ERP will instead focus on HCW’s compliance with compliance with universal precautions, competency, infection control practices, the nature of the work performed and techniques used by HCW. ERP may recommend adjustments of practice, restrictions, or other appropriate measures.
Minors' Access to STI and HIV Testing and Treatment
These summaries highlight key aspects of state laws governing the rights of minors to consent to testing and/or treatment for sexually transmitted infections (STIs) and HIV. Any such summary cannot capture the details and nuances of individuals state laws. Although roughly a third of the states permit health care providers to inform a minor's parents that their child is seeking STI-related services, none require it. Also, the law is fluid, and these summaries may not reflect recent legislative change in a particular state.
Every state in the country allows minors to consent to STI testing and care without parental approval, although a number of these set an age threshold for the right to consent without parental involvement. In these states, the minimum age ranges from 12 to 14 years of age.
As of the date of this posting, thirty-one states allow minors to also consent to HIV testing and treatment without parental approval.
HIV Testing
Unlike testing for most other infectious diseases, testing for HIV involves possible benefits as well as social, economic, and legal consequences that typically are not apparent or known to an individual considering testing. HIV-related testing is the gateway to health-preserving treatment; it also can be the basis of criminal prosecution for those who are sexually active, or relied on to exclude individuals who test positive for HIV from programs, employment, or insurance. Although state and federal laws prohibit much of this discrimination against people with HIV, the ability to enforce those rights usually depends on access to free legal services, which are increasingly limited and not available at all in roughly half of the states in the United States. Thus, the potential negative consequences of HIV testing at a particular time or location might inform an individual's decision of whether or when to get tested for HIV; or whether to test anonymously or through a "confidential" testing process that reports their test results and identifying information to the state but maintains the confidentiality of those results.
The American Medical Association has long defined informed consent as a process of communication between a patient and physician that results in the patient's authorization or agreement to undergo a specific medical intervention. Although informed consent is a legal concept rather than a medical one, many states use definitions of "informed consent" for purposes of HIV testing and medical procedures that in fact are inconsistent with the accepted legal definition, e.g., they do not require that an individual receive information or sometimes even notification that they are about to be tested for HIV. The Center for HIV Law and Policy (CHLP) accepts the legal and court-affirmed definition of informed consent; therefore, state protocols that call for "opt-out" testing (a patient is tested for HIV unless she/he objects) or that mirror general consent approaches are not counted as "informed consent" laws even in those instances where the state legislature has characterized their state law as requiring "informed consent." In short, CHLP does not consider or count laws that allow a patient's silence or general consent as granting authority to do confidential HIV testing as informed consent laws.
* Note: Although partner notification is not mandatory in Rhode Island, health care providers may inform third-parties with whom an HIV infected patient is in close and continuous exposure related contact, including, but not limited to a spouse and/or partner, if the nature of the contact, in the health care providers opinion, poses a clear and present danger of HIV transmission to the third-party, and if the physician has reason to believe that the patient, despite the health care provider's strong encouragement, has not and will not inform the third-party that they may have been exposed to HIV. See the Rhode Island General Laws, Title 23, Chapter 23-6.3, Section 23-6.3-10(b), Notification of disclosure.
Pre-test information and client-specific counseling tailored to the patient must be offered with HIV testing; information may be oral or written.
For positive results, post-test counseling must be given in person. Persons testing positive for HIV must also be provided with linkages and referrals to HIV-related counseling, health care and support.
Anonymous testing is available at designate anonymous testing sites.
Find the laws in a different state.
Copyright Information: CHLP encourages the broad use and sharing of resources. Please credit CHLP when using these materials or their content. and do not alter, adapt or present as your work without prior permission from CHLP.
Legal Disclaimer: CHLP makes an effort to ensure legal information is correct and current, but the law is regularly changing, and the accuracy of the information provided cannot be guaranteed. The legal information in a given resource may not be applicable to all situations and is not—and should not be relied upon—as a substitute for legal advice.